Diabetic Retinopathy Treatment in Oklahoma City
What Is Diabetic Retinopathy?
Dean McGee Eye Institute diagnoses and treats patients with diabetic retinopathy in Oklahoma City. Diabetic retinopathy is a progressive eye disease that develops when patients with diabetes have high enough sugar levels to damage blood vessels in the retina. Diabetic retinopathy may begin mild without any symptoms but can lead to blindness. The condition can develop in patients with Type 1 or Type 2 diabetes. The longer you have diabetes, the more likely you are to develop diabetic retinopathy. Early detection and treatment often helps patients save their sight.
Types of Diabetic Retinopathy
Diabetic retinopathy includes two types and four stages. The types of diabetic retinopathy include Nonproliferative Diabetic Retinopathy (NPDR) and Proliferative Diabetic Retinopathy (PDR). NPDR includes the early stages of diabetic retinopathy, while PDR is the most advanced form. The four stages of diabetic retinopathy include:
- Stage 1 – Mild nonproliferative diabetic retinopathy is characterized by small hemorrhages and/or microaneurysms, in the retina’s blood vessels. Fluid may start leaking into the retina, causing early macular swelling.
- Stage 2 – Moderate nonproliferative diabetic retinopathy includes increased damage to blood vessels, which interferes with the retina’s blood flow. The macula accumulates blood and other fluids in this stage, which begins to cause blurred vision.
- Stage 3 – Severe nonproliferative diabetic retinopathy is characterized by blocked blood vessels in the retina, leading to a significant decrease in blood flow. The body begins to receive signals to grow new blood vessels in the retina.
- Stage 4 – Proliferative diabetic retinopathy is the most advanced stage of the disease when new blood vessels are formed in the retina. These new blood vessels are very fragile and rupture easily, causing the vitreous gel to fill with blood. This can trigger a reduced field of vision, retinal detachment, blurry vision, and sometimes blindness.
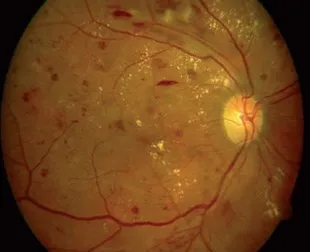
This photograph shows areas of hemorrhage and (yellow) exudates as seen in severe no proliferative diabetic retinopathy.
Symptoms of Diabetic Retinopathy
Diabetic retinopathy symptoms are typically hard to notice at first. As the condition progresses, diabetic retinopathy symptoms may include:
- An increasing number of floaters
- Blurred vision
- Blank or dark areas in your field of vision
- Poor night vision
- Colors appear faded or washed out
Diagnosing Diabetic Retinopathy
Diabetic retinopathy is diagnosed via a comprehensive eye examination during which your eyes will be dilated and the retina examined using an ophthalmoscope. You may also undergo a fluorescein angiogram, a test in which dye is injected into your arm and travels to the blood vessels in your eyes. A specialized camera takes photographs to determine if and where leaks and abnormal blood vessels are occurring.
What Are the Treatment Options for Diabetic Retinopathy?
The best treatment option for diabetic retinopathy is strict blood sugar control to reduce the risk of vision loss. If you require additional treatment for diabetic retinopathy, we offer:
Diabetic Retinopathy Treatment at the Dean McGee Eye Institute
For 45 years, the Dean McGee Eye Institute has been on the cutting-edge of eye care. Clinical trials are currently underway to develop new treatments for diabetic retinopathy. If you or a loved one are experiencing symptoms of diabetic retinopathy or you have been advised to see a retina specialist, our team of ophthalmologists specializing in retina and vitreous diseases would love to provide an eye examination to determine if treatment is needed. Call 405.271.1092 or 800.787.9014 to request your appointment.
Patient Testimonials
I was referred to the Dean McGee in 1989 or 90 when Dr. Kingsley was doing research on two lasers. There were other Drs. doing the research but he was my Doctor. Testing the argon and krypton on diabetic retinopathy was about a 4 month program. I am still able to see because of his work. Thank you Dr. Kingsley.
